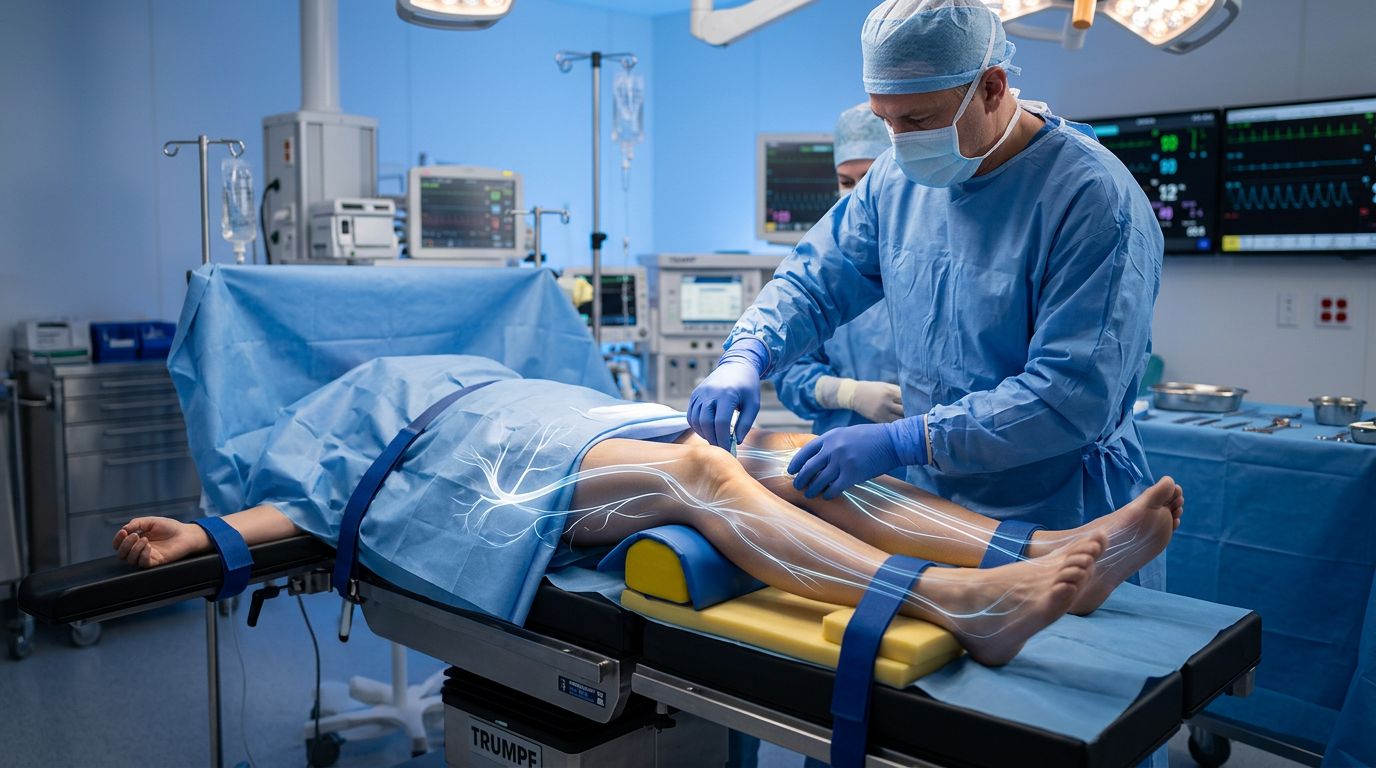
Florida Surgical Positioning Nerve Injuries and OR Liability
A routine operation can leave a patient with numb fingers, a weak foot, or pain that never should have started in the first place. When that happens, the problem may be more than a bad outcome, it may point to preventable harm in the operating room.
Florida surgical positioning nerve injury claims often turn on small details. How long did the case run? How were the arms and legs placed? Was padding used? Who checked the patient during surgery? If you are trying to sort out whether an injury was unavoidable or part of Florida OR liability, the records matter fast.
How a positioning mistake turns into nerve damage
During surgery, the patient cannot shift, speak up, or relieve pressure. That makes the operating table different from an ordinary bed. Small mistakes can turn into nerve compression, stretching, or loss of blood flow.
The risk rises when a case lasts a long time. It also rises when the body stays in one position without checks. Even a well-run operation can become risky if the patient has low body fat, diabetes, vascular problems, or a history of nerve issues.
The most common injuries involve nerves near bony areas. The elbow, shoulder, knee, and hip are all vulnerable. If an arm is stretched too far, the brachial plexus can be injured. If the elbow is pressed for too long, the ulnar nerve can be damaged. In leg surgery or procedures using stirrups, the peroneal nerve and sciatic nerve can also be affected.
These injuries often show up after anesthesia wears off. A patient may notice numbness, weakness, tingling, burning pain, or trouble lifting a foot. Some people think the symptoms are temporary. Sometimes they are. Other times, the damage lasts.
A positioning injury does not prove negligence by itself. The key question is whether the team took the steps a careful surgical team would have taken.
That is why these cases need more than a complaint of pain. They need a close look at what happened before, during, and after the procedure.
The surgical positions and nerves that get hurt most
Different procedures create different pressure points. A patient lying flat faces different risks than a patient in stirrups or a face-down position. The table below shows the patterns that come up most often.
| Position or setup | Common nerve involved | Typical result | Why it happens |
|---|---|---|---|
| Supine, arms extended on arm boards | Ulnar nerve, brachial plexus | Numbness in fingers, arm weakness, shoulder pain | The elbow or shoulder is compressed or stretched |
| Lithotomy, with legs in stirrups | Peroneal nerve, sciatic nerve | Foot drop, leg numbness, pain behind the knee | Stirrups or leg support press on the outer knee or stretch the leg |
| Prone, face down | Brachial plexus, ulnar nerve, sciatic nerve | Arm weakness, numb hands, leg pain | Pressure builds at the shoulder, elbow, or pelvis |
| Neck turned or arm spread too wide | Brachial plexus | Weakness across the shoulder and arm | Excess stretch affects the nerve bundle near the neck and shoulder |
The same injury can come from more than one cause. Hard stirrups, poorly placed arm boards, tight straps, or a failure to re-check position can all play a part. In longer cases, a single missed adjustment can matter more than people expect.
This is where the body acts like a closed circuit. If one part is trapped or stretched, the damage spreads outward. A patient may wake up with hand numbness, then learn later that a leg nerve was also affected. In other cases, the chart shows a complaint during surgery, but no one moved the limb or changed the setup.
Florida surgery cases also need to account for equipment. Retractors, padding, tables, and restraints can all create pressure. So can a rushed turnover or a staff shortage.
The location of the injury often points toward the source. That is one reason surgeons, anesthesiologists, nurses, and the hospital all have to be examined separately.
Where Florida OR liability can attach
Operating room liability rarely sits on one person alone. Several people may control different parts of the surgery, and each one can have a separate duty.
A surgeon may be responsible for the overall plan and for making sure the patient is positioned safely for the procedure. An anesthesiologist or nurse anesthetist may notice circulation or nerve concerns during the case. Circulating nurses often help with padding, limb placement, and checks. The hospital or surgery center may be responsible for staffing, equipment, policies, and training.
That matters because a claim can point to more than one failure. A nurse may have documented a problem and no one responded. A surgeon may have ordered an extreme arm angle. The facility may have used old stirrups or lacked a safe positioning policy. When those pieces line up, Florida OR liability can extend beyond one chart entry.
Hospitals can also face direct liability for their own conduct. If they failed to train staff, used unsafe equipment, or ignored repeated complaints about positioning practices, the issue is bigger than one bad move in one room. In some cases, the question is whether the facility created the conditions for harm.
In many cases, the most important question is who controlled the patient’s position, not who signed the consent form.
This is also where contracts matter. Some providers are hospital employees. Others are independent contractors. That difference can affect the way a claim is built, but it does not erase the underlying duty to provide safe care.
For a broader look at the legal framework, Avard Law’s Florida medical malpractice law guide explains the core elements that shape these cases.
What a Florida medical negligence claim must prove
Florida law uses the prevailing professional standard of care. The statute that sets out that rule is Florida’s medical negligence statute. In plain terms, the question is whether a reasonably careful provider would have done the same thing under similar circumstances.
That means a nerve injury claim needs proof of four things. First, there was a duty of care. Second, the care fell below the proper standard. Third, that failure caused the nerve injury. Fourth, the injury led to real losses.
The hard part is usually causation. A nerve injury can happen in surgery even when the team follows the rules. That is why the chart, the timing, and the medical opinions matter so much. A claim gets stronger when the records show a missed complaint, poor positioning, or a lack of checks.
The claim also gets stronger when the injury matches the position. For example, foot drop after prolonged lithotomy positioning may point toward peroneal nerve compression. Arm weakness after a long case with extreme arm extension may point toward brachial plexus injury. The pattern has to make medical sense.
A lot of people expect a doctor to admit fault. That almost never happens. What usually matters is the paper trail. Did the records show the patient was numb, weak, or in pain during recovery? Did anyone document why the position was changed or not changed? Did the team notice the signs early enough to act?
The claim does not need drama. It needs proof.
What to do in the first days after you notice symptoms
The first week matters because records fade and memories get fuzzy fast. If you woke up with numbness, weakness, or foot drop, start gathering the facts right away. Avard Law’s first week checklist for Florida medical malpractice victims is a good place to see how early action protects a claim.
Start with the basics:
- Tell the surgeon, recovery staff, or nurse about the symptoms right away.
- Ask for the complete record set, not only the discharge summary.
- Save the operative report, anesthesia record, nursing notes, and medication records.
- Write down when the symptoms started and how they changed.
- Keep photos of bruising, skin marks, braces, or visible swelling.
- Follow up with the specialists you were told to see.
The most useful records often sit outside the surgeon’s note. Post-op nursing notes, physical therapy records, and anesthesia records can show when the injury began and whether anyone reacted to warning signs. If a nurse noted a complaint but no one changed the positioning, that can be important.
Do not wait for someone to volunteer the truth. Medical charts may give the answer, but only if they are preserved early. A patient who waits months can lose details that would have been clear in the first week.
A legal review also helps decide whether the issue is positioning, a surgical tool, swelling, or something else entirely. That distinction matters. A strong claim needs the right target.
Damages and deadlines in Florida
A nerve injury can affect work, sleep, driving, walking, and daily tasks. Some patients need therapy, braces, injections, repeat surgery, or long-term pain care. Others lose income because they can no longer do the same job.
That is why damages in these cases can include more than medical bills. They may include future treatment, lost wages, reduced earning power, home help, and pain and suffering. If the nerve damage is permanent, the cost can spread over years.
Timing matters just as much. Florida medical negligence claims have short deadlines, and waiting too long can block a case even when the injury is serious. The clock can depend on when the injury was discovered or should have been discovered, so it is risky to guess.
The deadline issue is one reason early record collection matters. Once the time window starts closing, the case gets harder to prove and harder to file. That is especially true when the injury first looked like a normal recovery problem.
If the symptoms improve, that does not always mean the claim is over. Some nerve injuries get better. Others leave lasting weakness or pain. The full picture may take weeks or months to develop, but the legal clock does not wait for the body to catch up.
Conclusion
A surgical positioning nerve injury can look like a random complication, but the details often tell a different story. The position, the padding, the length of the case, and the response to early symptoms all matter.
When those details show a missed safety step, Florida OR liability may reach the surgeon, the anesthesia team, the nurses, and the facility itself. The sooner the records are preserved, the clearer the case becomes.
If you are dealing with numbness, weakness, or foot drop after surgery, treat it as a record-keeping problem as much as a medical one. The chart often decides what happens next.