Florida Fetal Monitoring Negligence and Birth Injury Liability
Labor can turn in minutes. A monitor strip can show trouble long before anyone in the room feels panic.
When staff miss those warning signs, a child can suffer lasting harm. Fetal monitoring negligence can lead to oxygen loss, brain injury, cerebral palsy, stillbirth, or death.
Florida families often do not know what went wrong until after delivery. The chart, the timing, and the response from the delivery team usually tell the story.
What fetal monitoring negligence looks like in a Florida delivery room
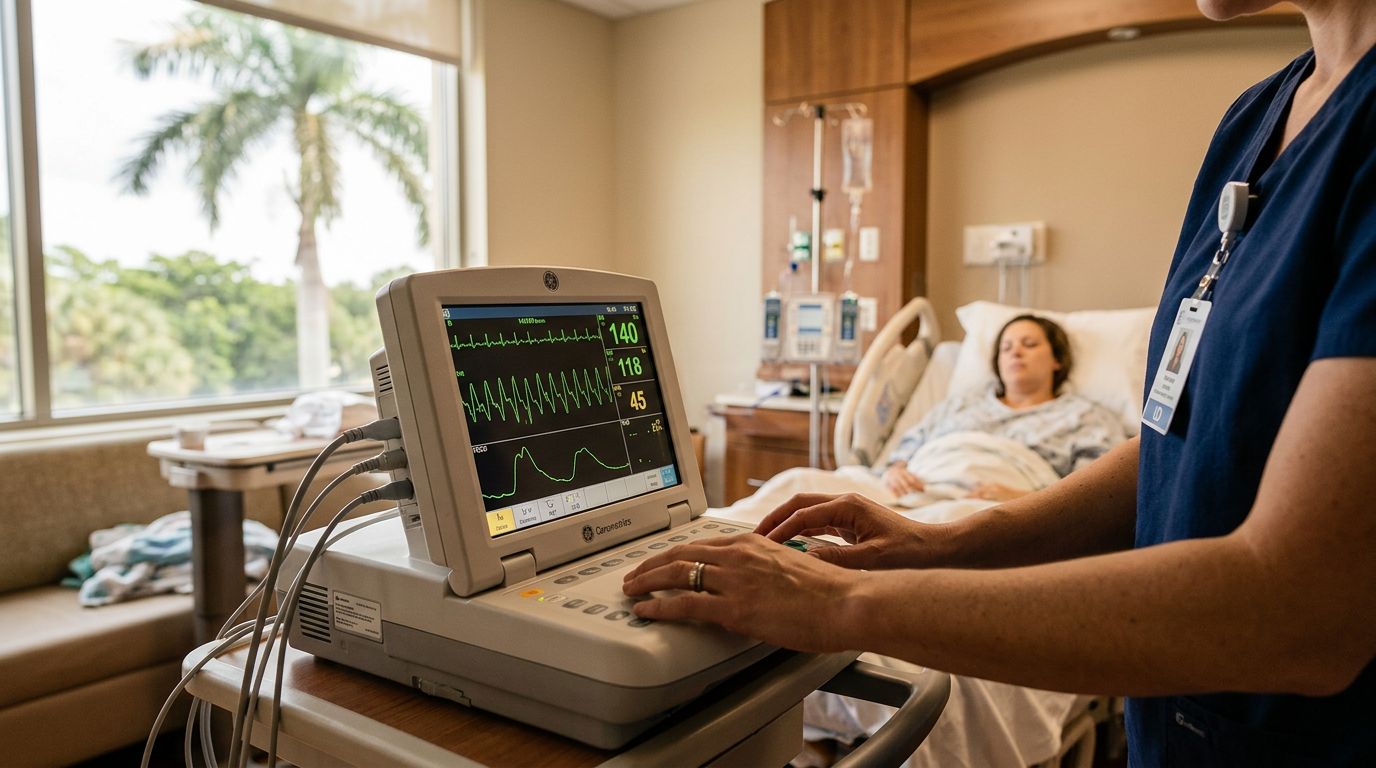
During labor, the medical team watches the baby’s heart rate and the mother’s contractions. That can happen with belts on the belly or, in some cases, internal sensors.
The goal is simple. The staff should spot distress early enough to act. A careful team watches the tracing, notices changes, and responds fast when the baby looks stressed.
Negligence happens when that process breaks down. A nurse may miss an abnormal pattern. A doctor may not come when called. A delivery team may wait too long to move from monitoring to intervention.
Common failures include reading the strip the wrong way, ignoring repeated alarms, or using monitoring equipment the wrong way. Poor handoffs can also cause trouble. One nurse may see a bad tracing, but the next nurse may never hear about it.
A bad result alone does not prove malpractice. Babies can have complications even when the team does everything right. Still, repeated errors, ignored signs, and slow responses can point to a breach of the standard of care.
These cases often fall under broader medical negligence claims. Many fit the kind of harm described in examples of medical malpractice, because the issue is not the outcome alone. The issue is whether the delivery team acted as a careful team should have acted.
Warning signs on the monitor that staff should not ignore
Not every unusual tracing means someone made a legal mistake. Some patterns can appear and clear on their own. Others need immediate action.
The problem starts when a troubling pattern keeps getting worse. In labor, the monitor is often the clearest warning the team gets.
| Monitor finding | Why it matters |
|---|---|
| Repeated drops in heart rate after contractions | Can point to cord compression or reduced oxygen |
| A long heart rate drop that does not recover | May show the baby is not bouncing back |
| Little or no beat-to-beat change | Can be a sign of fetal stress |
| A tracing that gets worse over time | May call for fast escalation, not more waiting |
A nurse or doctor does not need to guess at every tracing. Still, they do need to pay attention to the trend. One isolated dip may not mean much. A pattern that keeps changing tells a different story.
Families sometimes hear words like “non-reassuring fetal status” or “fetal distress.” Those terms matter because they tell the team that the baby may not be getting enough oxygen. If the tracing is getting worse, the response should get faster.
That response may include changing the mother’s position, stopping a medication, giving oxygen if appropriate, calling the doctor right away, or preparing for a C-section. Waiting without a plan can be the wrong move.
A delivery room is not a place for slow reactions. The baby’s brain and organs do not wait while people debate what the strip means.
How missed distress turns into a birth injury
A baby who does not get enough oxygen can be injured fast. The brain is the main concern because brain tissue is sensitive to oxygen loss.
That is why timing matters so much. If the strip shows distress and the team waits too long, the injury can grow worse while everyone hopes the problem will settle on its own.
A delayed C-section is one common example. If the monitor shows signs of danger and the team does not act in time, the baby may move from distress to lasting harm. The same risk exists when nurses fail to pass along the warning, or when a doctor is called and does not respond.
The injury can be severe. Families may face:
- brain damage
- oxygen deprivation
- seizures
- cerebral palsy
- developmental delay
- stillbirth
- newborn death
Mothers can also be harmed. A delayed emergency response may lead to bleeding, infection, or complications tied to the delivery itself. In some cases, the same delay harms both mother and child.
These cases are painful because the chart often looks ordinary at first glance. A few time stamps, a short note, or a delayed call can hide a long gap in care. When that gap lines up with the baby’s decline, the record starts to matter a great deal.
What has to be proven in a Florida malpractice claim
A Florida fetal monitoring negligence claim is built on four core points. Each one has to be supported by proof.
| Legal element | What it means in plain English |
|---|---|
| Duty | The provider had a duty to care for the mother and baby |
| Breach | The provider fell below accepted medical care |
| Causation | The mistake caused or worsened the injury |
| Damages | The child or mother suffered real harm and losses |
That table looks simple. The real case is not simple at all.
The strongest evidence often comes from the fetal monitor strip, nursing notes, doctor notes, medication records, and delivery times. Those records show who saw what and when they saw it. If the tracing became dangerous at 2:10 p.m. and the doctor was not called until 2:45 p.m., that time gap can matter.
Expert medical review is also key. A qualified expert can compare the hospital’s actions to accepted practice. The question is direct. Would a careful provider have seen the danger and acted sooner?
The defense often argues that the injury happened anyway. They may say the baby was already in trouble or that no intervention could have changed the result. That is why the timeline matters so much. If the team had a window to act and missed it, the case becomes stronger.
Birth-related harm is one of the clearest examples of serious medical negligence. It fits within the kinds of medical malpractice claims families hear about after a bad hospital experience. The legal fight is usually about proof, not emotion, and proof starts with the records.
Florida malpractice rules that shape these cases
These claims are usually treated as medical malpractice cases, so they do not move like ordinary injury claims. Florida uses special pre-suit steps, and families have to move within the legal time limits.
That matters because delay can hurt the case. Records can get harder to obtain. Staff members can change jobs. Memories fade. Meanwhile, the legal clock keeps moving.
The process often starts with a close record review and a medical expert. Before a lawsuit can move forward, the facts need to support the claim. That review helps identify which providers were involved, what they knew, and when they knew it.
In a birth injury case, the defendants may include more than one person. Nurses, obstetricians, residents, anesthesiologists, and the hospital itself may all play a role. Each person’s actions have to be measured against the care that should have been given.
Hospital liability can also matter when the nurse or staff member was acting within the scope of employment. That is one reason the delivery-room timeline is so important. It can show who had control, who had authority, and who failed to respond.
Florida law does not reward guesswork. It rewards evidence. Families who suspect a monitoring error should act quickly, because the strongest cases are built while the records are still fresh and the details can still be checked.
What compensation may cover after a birth injury
A birth injury can change a family’s finances in a matter of days. The first hospital bill is often only the beginning.
Long-term care may include therapy, specialist visits, medications, surgery, mobility equipment, and home nursing. Some children also need early intervention, assistive devices, or special education support for years.
Parents may lose work time while they care for the child. They may need a different car, home changes, or travel to specialists in another city. Those costs add up fast.
In a Florida claim, compensation may cover medical expenses, future care, lost income, pain and suffering, and other losses tied to the injury. If the injury leads to a wrongful death claim, the law may also allow recovery for that loss.
The law looks at the full cost of the harm. It does not stop at the delivery room. A serious injury affects the child’s future, and that future has a real value in court.
When to contact a Florida birth injury lawyer
If something felt wrong during labor, the first step is to get answers. Ask for the medical records. Ask for the fetal monitor strip. Ask for the delivery timeline.
A lawyer who handles these cases can help preserve that evidence before it disappears into a larger chart request. The attorney can also review the records with medical experts and look for gaps in care, bad timing, and missed warnings.
Families often speak with Florida birth injury lawyers when they want a clear look at what happened in the delivery room. That review can show whether the case points to a preventable injury, a communication breakdown, or a delayed response that should have happened sooner.
The earlier that review starts, the better. Monitor strips, notes, and orders tell a story, but only if someone reads them before they are lost in the noise of discharge papers and follow-up visits.
Conclusion
A monitor strip is supposed to buy time. When staff ignore what it shows, that time can disappear.
For Florida families, birth injury liability often comes down to a few hard facts. What did the tracing show, who saw it, and how fast did the team respond? Those answers can decide whether the injury was unavoidable or the result of fetal monitoring negligence.
When a delivery room stays calm for too long, the chart may hold the truth. In these cases, the record is often the clearest path to accountability.