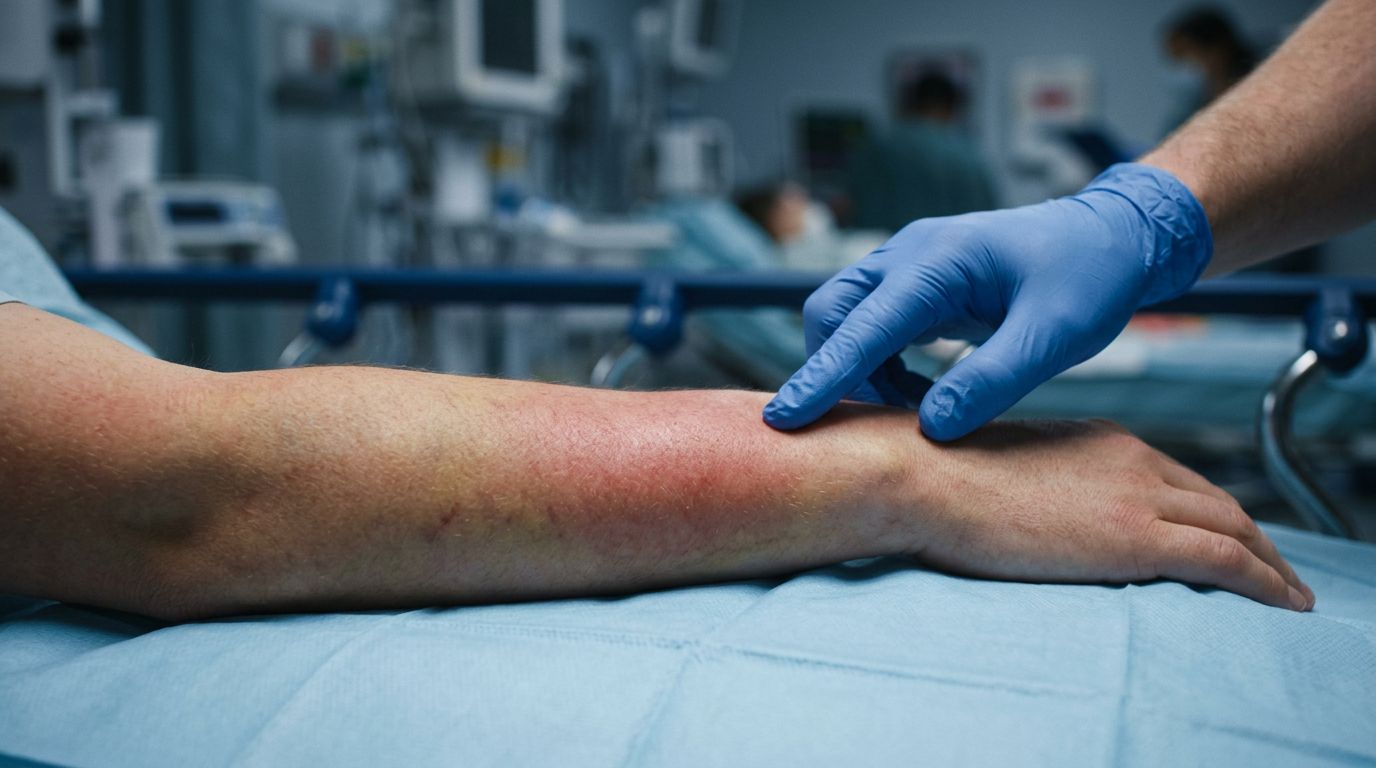
Florida Necrotizing Fasciitis Misdiagnosis and ER Warning Signs
A missed soft-tissue infection can turn dangerous fast. With necrotizing fasciitis, the first signs may look like a routine skin problem, but the infection can spread beneath the surface in hours.
That is why ER warning signs matter so much. If pain, swelling, or redness worsens after a cut, wound, surgery, or injection, the details deserve close attention, especially when the first visit ended with a quick discharge.
Early warning signs that should send you back to the ER
Necrotizing fasciitis often starts with symptoms that seem minor. The CDC notes that early diagnosis is hard because the first signs can look like other infections, but certain symptoms should raise concern fast. See the CDC clinical guidance on necrotizing fasciitis for the medical warning signs doctors are told to watch for.
Pain that seems far worse than the wound looks is a major red flag.
Watch for these changes:
- Severe pain out of proportion to the visible injury
- Redness or swelling that spreads quickly
- Fever, chills, or vomiting
- Skin color changes, including purple, gray, or black areas
- Blisters, drainage, or a foul smell
- Numbness or loss of feeling near the wound
The CDC also lists severe pain, skin changes, and fast spread as warning signs on its public overview of the disease. The CDC overview of necrotizing fasciitis is a useful reference if you want to compare symptoms with what you saw in the ER.
A key point is this, necrotizing fasciitis does not always look dramatic at first. A wound can seem small while the damage spreads under the skin.
Why necrotizing fasciitis gets missed in the ER
ER teams see a lot of skin complaints. Most are not emergencies, so a serious infection can get labeled as cellulitis, an abscess, an allergic reaction, or a simple wound problem.
That is where necrotizing fasciitis misdiagnosis often starts. The first exam may focus on what the skin looks like, while the deeper pain and speed of worsening get missed.
Several things make the mistake easier:
- Early symptoms can look mild.
- Pain may seem vague or hard to measure.
- Lab results may not tell the full story at first.
- The infection can spread before skin changes become obvious.
Florida patients can face added risk when injuries follow beach cuts, outdoor wounds, recent surgery, or delayed care for a skin break. The setting matters less than the symptom pattern, though. Rapid change is the warning sign that should not be brushed aside.
If the pain keeps climbing, or the redness keeps moving, the visit should not end with reassurance alone.
When a missed diagnosis may become medical malpractice in Florida
Not every bad outcome is malpractice. Florida medical negligence claims usually turn on whether the provider failed to meet the accepted standard of care and that failure caused harm.
In a necrotizing fasciitis case, the problem may be:
- ignoring severe pain that did not fit the exam
- failing to order more testing
- not consulting surgery soon enough
- sending the patient home too early
- missing a clear change in condition after a return visit
For a broader look at how these claims work, review the Florida medical malpractice law guide. The legal issue is not just whether the infection was hard to see. It is whether the ER response matched what a careful provider should have done.
Florida also uses strict timing rules, and the Florida malpractice deadlines can matter before a case is fully built. That makes early record review important.
A missed diagnosis case often turns on the chart. If the notes show worsening pain, spreading redness, fever, or repeat visits, the record may tell a story that the discharge papers do not.
What to do after a suspicious ER visit
If the wound gets worse after the ER visit, move fast. Do not wait for the pain to “settle down” on its own.
- Return for urgent care or another ER visit if symptoms are spreading.
- Ask for all records from every visit, including triage notes, labs, and discharge papers.
- Take photos of the wound and any skin changes each time you notice a shift.
- Write down the timeline of pain, fever, swelling, and any missed warnings.
- Keep names and dates for every doctor, nurse, and facility involved.
That paper trail matters. It helps a doctor see what changed, and it helps a lawyer see whether the care fell short.
Conclusion
Necrotizing fasciitis can begin like an ordinary infection, then turn into a medical emergency before the skin tells the full story. The biggest warning sign is often the one patients describe first, pain that is worse than it should be.
If an ER visit ended with a diagnosis that did not fit the symptoms, the records should be reviewed quickly. In Florida, timing matters, and a missed infection can leave a clear trail if the chart is read closely.